Rolling Forward - BDNF
Complex Movement, BDNF, and Rebuilding the Injured Brain
Most people think of exercise as something you do for your heart. Burn calories. Lower blood pressure. Improve endurance. These are real and meaningful benefits. But they describe only part of what movement does to the body — and almost none of what it does to the brain.
Movement is not just a cardiovascular event. When it demands attention, timing, adaptation, and learning, it becomes a neurological event as well. And at the center of that process is a protein called brain-derived neurotrophic factor, or BDNF.
What BDNF is, and Why It Matters
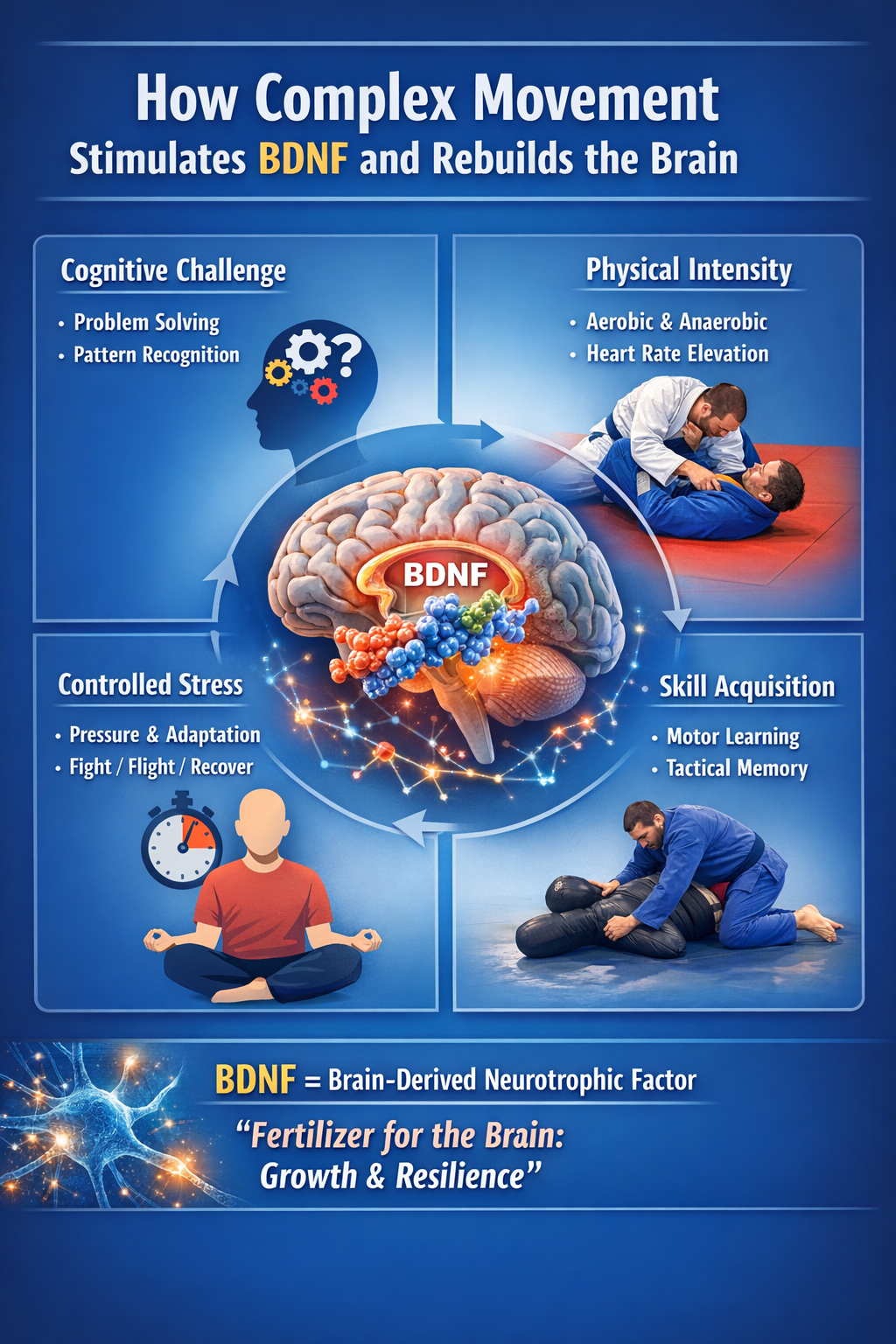
BDNF is a member of the neurotrophic family — signaling proteins that regulate the survival, growth, and maintenance of neurons. It is often described, informally, as "fertilizer for the brain," and while that metaphor flattens a complex biology, it captures something real. BDNF supports synaptic plasticity, the process by which neuronal connections are strengthened or pruned in response to experience, and it plays a particularly prominent role in the hippocampus, the region most closely associated with memory formation, spatial navigation, and emotional regulation.
Lower BDNF levels have been associated, in both preclinical and clinical research, with depression, cognitive decline, and neurodegenerative conditions including Alzheimer's disease. Higher levels correlate with improved learning capacity and better mood regulation. After traumatic brain injury (TBI), BDNF signaling can be disrupted at multiple levels — including expression, transport, and receptor sensitivity — making the question of how to support its recovery biologically meaningful, not merely theoretical.
It is worth being precise here: BDNF is one pathway among many involved in neuroplasticity. It is neither a cure nor a complete mechanism on its own. But it is one of the best-studied molecular markers linking physical effort, learning, and adaptive brain change, which is why it anchors this discussion.
Exercise, Aerobic Load, and the BDNF Response
The relationship between aerobic exercise and BDNF elevation is among the more robustly replicated findings in exercise neuroscience. Studies in both animal models and human subjects have documented acute increases in circulating BDNF following moderate-to-vigorous aerobic activity, with particularly strong effects in the hippocampus. The mechanisms appear to involve increased cerebral blood flow, upregulation of the BDNF gene via transcription factors activated by muscle contraction (including FNDC5/irisin), and autonomic nervous system engagement.
What is less frequently acknowledged is that not all movement stimulates the brain in the same way. There is a meaningful neurological difference between repetitive, predictable motion and motion that requires constant adaptation. Jogging on a treadmill at a steady pace elevates heart rate and generates BDNF — and that has genuine value. But jogging while simultaneously solving shifting physical problems under real-time pressure engages a substantially different neural profile. The prefrontal cortex, anterior cingulate, motor cortex, cerebellum, and limbic structures are recruited in different combinations depending on the cognitive and emotional demands of the movement itself.
This distinction matters because BDNF expression is stimulated not only by exertion but by learning. Research in rodent models has shown that environmental enrichment, skill acquisition, and novelty independently upregulate hippocampal BDNF, even when aerobic demands are held constant. The implication is that movement which combines cardiovascular stress with genuine cognitive engagement may produce a more comprehensive neuroplastic stimulus than either element alone.
Brazilian Jiu-Jitsu as a Neurological Training Environment
Brazilian Jiu-Jitsu is often described as physical chess. That description is more neurologically accurate than poetic. During a live roll — a training match — the heart rate enters moderate-to-high intensity zones sufficient to drive aerobic BDNF signaling. Simultaneously, the brain is required to process three-dimensional spatial orientation, anticipate an opponent's intent from subtle kinesthetic cues, retrieve and sequence technical movement patterns under time pressure, regulate fear and frustration, and make rapid tactical decisions when conditions change.
These demands recruit the hippocampus (spatial mapping, pattern storage), the prefrontal cortex (decision-making, emotional inhibition), the motor cortex (precise motor output), and the cerebellum (timing, proprioception, error correction) — often in parallel. The layering of cardiovascular load with high-stakes cognitive processing may represent an unusually potent combination for BDNF stimulation. It should be stated clearly that this is a mechanistically plausible hypothesis, not a conclusion drawn from BJJ-specific clinical trials. No randomized controlled trial has yet directly measured BDNF outcomes in Brazilian Jiu-Jitsu practitioners compared to matched controls. The inference is drawn from the known neurological demands of the sport and extrapolated from research on complex motor skill learning more broadly.
Where the evidence is stronger is in the general literature on skill-based motor learning. Studies examining musicians, dancers, and athletes in sports with high coordinative demands have documented neuroplastic changes including increased hippocampal volume, enhanced white matter integrity, and improved executive function compared to sedentary controls. These changes appear linked to the duration and complexity of training, not simply to fitness level — suggesting that the cognitive content of movement matters independently of its aerobic component.
Adaptive Stress, Controlled Challenge, and the Nervous System
Brazilian Jiu-Jitsu also introduces a specific quality of stress that is worth examining carefully. During a roll, you are placed in uncomfortable positions. Breathing becomes restricted. A larger opponent applies sustained pressure. The sympathetic nervous system activates. The experience can be genuinely unpleasant — and it can be highly instructive.
The critical variable is structure. This stress is bounded, consensual, and recoverable. You tap. You reset. The nervous system activates and then returns to baseline, repeatedly, within a single session. That cycle of sympathetic activation followed by parasympathetic recovery is biologically distinct from the chronic, low-grade stress associated with suppressed BDNF expression, elevated cortisol, and impaired hippocampal neurogenesis. Research on hormetic stress — the principle that brief, controlled physiological challenges can enhance adaptive capacity — supports the idea that repeated exposure to tolerable adversity, when followed by adequate recovery, may strengthen neuroplastic signaling rather than suppress it.
For someone rebuilding after TBI, this distinction is clinically relevant. Recovery does not mean avoiding all challenge. The nervous system, like muscle tissue, responds to graded loading. The goal is to reintroduce structured, tolerable challenge in a way that promotes adaptation without overwhelming the system. Complex movement environments like BJJ offer exactly that architecture, provided the training is coached intelligently and exposure is progressed gradually. Importantly, not all TBI recoveries are alike, and the appropriateness of high-intensity, contact-based exercise must be individualized under medical supervision.
Acute BDNF Spikes Versus Long-Term Structural Change
One of the more important nuances in this literature is the difference between an acute BDNF response and lasting structural neuroplasticity. A single bout of vigorous exercise produces a measurable, transient increase in circulating BDNF, peaking roughly 15 to 30 minutes post-exercise and declining toward baseline within an hour or two. This acute spike is real, but it does not, on its own, produce lasting change.
Long-term structural plasticity — the kind associated with durable improvements in memory, executive function, and cognitive resilience — requires sustained training over weeks and months. Animal studies suggest that chronic exercise upregulates BDNF at a baseline level, increases the density of BDNF-responsive synapses, and promotes hippocampal neurogenesis (the generation of new neurons in the dentate gyrus), a process that has been linked to improved spatial memory and emotional regulation. Human imaging studies have documented measurable hippocampal volume increases in older adults following six months of aerobic exercise — changes correlated with BDNF levels and memory performance.
The takeaway is straightforward but easily misread: the acute response matters because it opens a window of heightened synaptic plasticity. What you do in the hours following training — sleep, moderate cognitive engagement, adequate nutrition — may influence how much of that potential is converted into durable structural change. Consistency matters more than intensity alone. A single transformative session does not rebuild a brain. The neuroplastic effects of complex movement are cumulative.
Sleep: The Consolidation Window
No discussion of BDNF-mediated plasticity is complete without addressing sleep. The relationship between exercise-induced BDNF signaling and sleep is bidirectional and deeply intertwined. Aerobic exercise has been shown to improve both sleep architecture and slow-wave sleep duration — the stage most closely associated with memory consolidation and the clearance of metabolic waste products (including amyloid-beta) via the glymphatic system.
During slow-wave and REM sleep, the brain replays recently encoded experiences, stabilizing them from labile, short-term traces into more durable long-term representations. BDNF plays a facilitating role in this consolidation process: sleep deprivation attenuates BDNF expression in the hippocampus, impairing the very plasticity that daytime training is designed to stimulate. For someone recovering from TBI — a population with significantly elevated rates of sleep disturbance — this interaction is not peripheral. It is central. Optimizing sleep quality is not a lifestyle recommendation added onto a rehabilitation program; it may be a prerequisite for that program to work.
The practical implication: training that is intense enough to drive genuine BDNF signaling but is not followed by adequate sleep may deliver a stimulus without a consolidation window — like planting a seed and failing to water it.
The Broader Neurochemical Cascade
BDNF does not operate in isolation. Vigorous, skill-based training also releases dopamine (reinforcing learning and motivation), serotonin (supporting mood regulation and anxiety reduction), endorphins (modulating pain and generating positive affect), and noradrenaline (sharpening attention and encoding emotional salience). These neurotransmitters interact with BDNF signaling pathways, and their combined release during and after intense training likely amplifies the learning and mood effects beyond what any single molecule could produce.
The subjective clarity many practitioners report following training is not imaginary, nor is it merely placebo. It reflects a neurochemical cascade that supports both cognitive readiness and emotional regulation. For individuals with TBI — who commonly experience depression, anxiety, fatigue, and cognitive fog — this post-training neurochemical window may offer a meaningful, if temporary, relief that also happens to be therapeutic.
Cognitive Reserve, Aging, and the Cost of Simplification
Cognitive reserve refers to the brain's capacity to tolerate injury or degeneration before functional impairment becomes apparent. It is built, over a lifetime, through education, intellectual engagement, social connection, and — increasingly, the evidence suggests — complex physical activity. People with greater cognitive reserve show delayed onset of dementia symptoms even when pathological burden is equivalent to those with fewer symptoms. This reserve is not fixed; it is dynamically maintained or eroded depending on the demands placed on the brain.
As people age — or recover from injury — there is an instinct to simplify. To reduce novelty. To avoid discomfort. To choose the easier movement, the quieter environment, the more predictable routine. This instinct is understandable. It is also, from a neurological standpoint, potentially counterproductive. The brain requires adaptive demand to maintain its architecture. Simplified, low-challenge movement may preserve cardiovascular fitness while offering relatively little stimulus for the kind of synaptic refinement that supports cognitive resilience.
Complex movement disciplines — those that require memory, timing, spatial reasoning, emotional regulation, and rapid decision-making under pressure — may serve a protective function precisely because they impose the kind of demand the brain needs to stay adaptable. This applies not only to BJJ but to other cognitively demanding movement practices: classical dance, which combines precise motor sequencing with musical timing and spatial awareness; rock climbing, which requires problem-solving and fear regulation under physical stress; and certain racket sports, which demand anticipatory cognition and rapid visual-motor integration. The common feature is not the sport itself, but the cognitive load embedded in the movement.
A Note on Safety in the TBI Population
Any discussion of Brazilian Jiu-Jitsu in the context of brain injury recovery must be direct about risk. BJJ is a contact sport that involves grappling, positional control, and submission attempts, some of which involve cranial and cervical pressure. The risk of further head injury — particularly in sparring situations with resistive partners — is not trivial.
For individuals with a history of TBI, the potential benefits of complex movement training must be weighed carefully against the risk of re-injury. Technical drilling, positional flow rolling with cooperative partners, and graduated exposure under expert coaching represent a substantially different risk profile than open sparring. Medical clearance, individualized pacing, and transparent communication with coaching staff are non-negotiable. The goal of applying these principles is neurological stimulation, not athletic competition. Those are different training objectives, and they require different program design.
Scientific Integrity: What We Know, What We Infer, and What Remains Theoretical
The following distinctions are offered in the interest of honest science communication:
What is well-established: Aerobic exercise acutely elevates BDNF in humans. Chronic exercise training produces lasting upregulation of BDNF, promotes hippocampal neurogenesis in rodents, and is associated with measurable hippocampal volume changes in humans. Sleep consolidates exercise-induced synaptic plasticity. Chronic stress suppresses BDNF; short-duration, recoverable stress can enhance adaptive signaling. Skill-based motor learning independently drives hippocampal plasticity beyond what aerobic exercise alone produces.
What is strongly suggested but not directly proven in BJJ populations: That the combined aerobic and cognitive demands of live grappling practice produce a broader or more potent neuroplastic stimulus than matched aerobic exercise alone. That regular BJJ training improves executive function, emotional regulation, and attentional control. That the structured stress architecture of training — activation, tap, reset, recovery — produces adaptive hormetic effects. These claims rest on plausible mechanistic inference from adjacent research, not on BJJ-specific clinical trials.
What remains theoretical or extrapolated: The specific magnitude of BDNF elevation during BJJ. The degree to which any observed cognitive or emotional benefits in practitioners are attributable to BDNF versus other neurochemical or psychosocial mechanisms. The optimal training parameters (frequency, intensity, technical-to-sparring ratio) for neuroplastic benefit in TBI recovery. Claims in this domain should be held proportionally to the evidence that supports them.
Suggested Research Areas
The following study types would most meaningfully advance or challenge the claims made in this article:
1. Randomized controlled trials comparing serum and cerebrospinal fluid BDNF levels in individuals assigned to BJJ training versus matched aerobic exercise (e.g., cycling at equivalent heart-rate zones) over 12 to 24 weeks, with neuropsychological outcome measures. This would directly test whether the cognitive complexity of grappling produces additive neuroplastic benefit beyond aerobic load alone.
2. Longitudinal neuroimaging studies (fMRI, DTI) in TBI patients enrolled in complex movement rehabilitation programs, measuring hippocampal volume, white matter integrity, and functional connectivity changes over time compared to standard-of-care comparators.
3. Sleep-stratified analyses in exercise-BDNF studies: examining whether sleep quality and duration moderate the conversion of acute BDNF elevations into durable cognitive gains. This would test the consolidation hypothesis directly.
4. Mechanistic studies using resistance to acute stress as a dependent variable: does regular participation in structured, recoverable-stress environments (grappling, competitive sport) alter HPA-axis reactivity, vagal tone, or baseline BDNF in ways that predict cognitive resilience?
5. Comparative studies across cognitively demanding movement disciplines (BJJ, classical dance, climbing, tennis) matched for aerobic intensity, examining differential effects on executive function and hippocampal markers — this would help isolate the contribution of movement complexity and novelty from cardiovascular load.
The brain does not heal through passivity. It heals through intelligent, graduated challenge — delivered consistently, followed by adequate recovery, and supported by honest science about what we know and what we are still learning. Complex movement, when properly understood and carefully applied, may represent one of the most underutilized tools in cognitive rehabilitation. The mat is not a clinic. But for some, it may be part of the treatment.